SPONSORED byTokuyama
By Mark Kleive, DDS
The biggest challange with most large antierior composite restorations is achieving an invisible margin between the restorative material. The factors that influence esthetic success include:
- The amount of natural tooth structure loss
- The ability of the restorative material to mimic the remaining tooth structure
- The restoration's polish over time
- The amount of staining that exists as part of the patient's lifestyle
With specific techniques, every clinician can improve the esthetic outcomes of their anterior composite restorations.
In this case, the patient had esthetic concerns regarding the discolored filling on his tooth #9. While the patient had other evidence of occlusal dysfunction, the patient's primary concern was an improved esthetic outcome, and that became the primary goal of the restorative therapy.
"The biggest challange with most large antierior composite restorations is achieving an invisible margin between the restorative material."
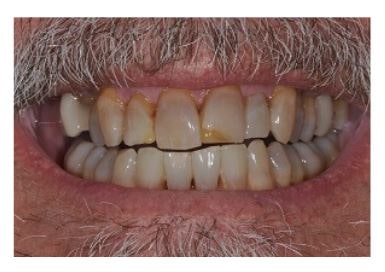


Preoperative view shows a previous Class IV restoration with poor esthetics, poor contours, and marginal breakdown.
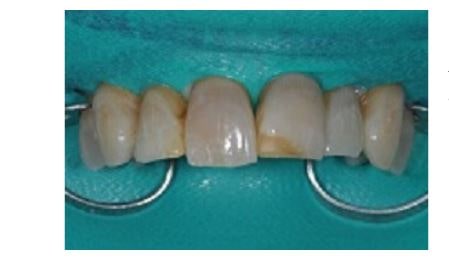
Rubber dam is placed to isolate the teeth against contamination and improve access.
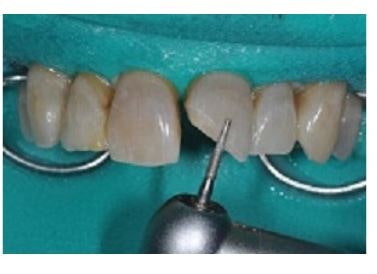
A 40-µm diamond is used to smooth out the jagged margins of the tooth, and create a smooth bevel at least 2 mm beyond the fracture line. This softens the edges and rounds off the fractured enamel prisms.
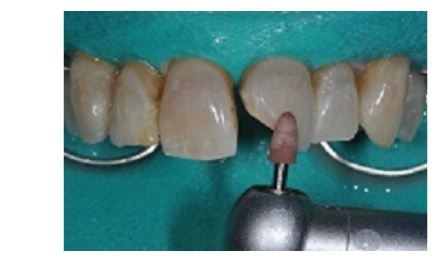
A silicone polisher was used to provide the final smoothing of the preparation.
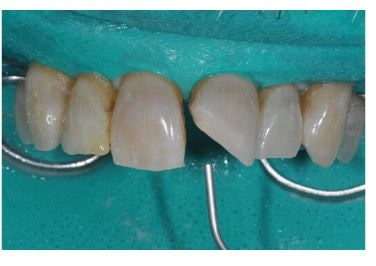
Here is the situation after the silicone polisher and sandblasting with 50-µm aluminum oxide. When making the bevel, it is best done in a sun-burst manner. This ensures that the light reflection in the finished restoration occurs in a wavy, not straight line.
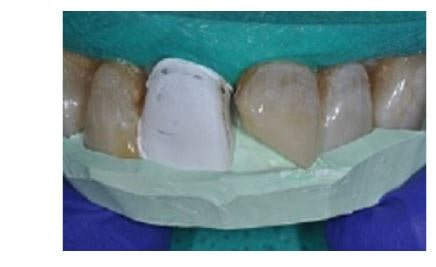
The silicone key is tried and, if needed, adjusted to ensure that the incisal edge is just visible.
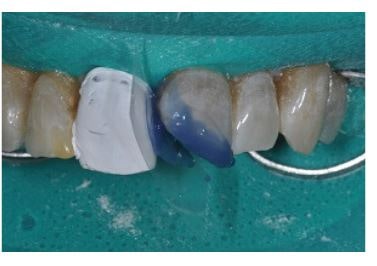
The tooth is etched while the adjacent teeth are protected, using polytetrafluoroethylene tape. Selective etching is advised, and in this case, 37% phosphoric acid was used for 30 seconds on the enamel and 15 seconds on the dentin.
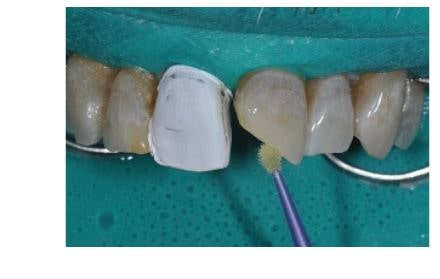
Multiple coats of bonding agent are applied (Bond Force, Tokuyama Dental America; Encinitas, CA) and after 30 seconds, air is blown to let the solvent evaporate and for thinning the bonding agent. It is applied on all the area that has been etched and not only on the fractured margin.
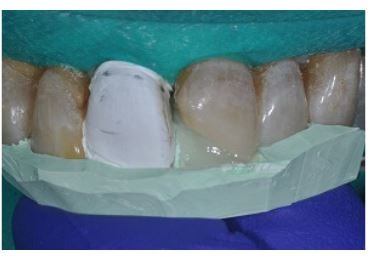
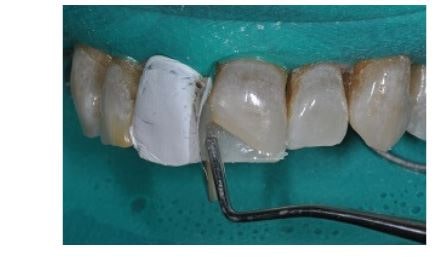
The palatal wall is created (MW Estelite Omega, Tokuyama Dental America), using the sectional matrix to maintain the predetermined shape.
The proximal wall is created using a vertical sectional matrix (EA2, Estelite Omega, Tokuyama Dental America). This technique maintains the appropriate shape of the proximal wall in both the labial/lingual and incisal/gingival dimensions.
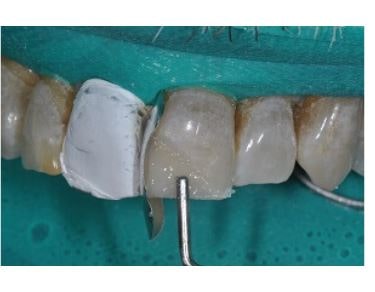
A gel is placed for oxygen inhibition, and the restoration is cured after the enamel layer (EA2, Estelite Omega, Tokuyama Dental America) is placed.
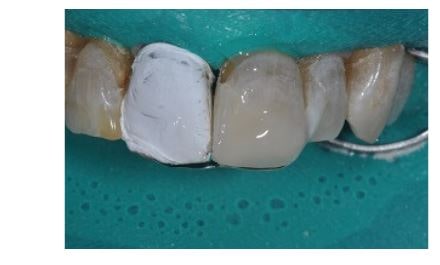
The dentin material is shaped to attain primary and secondary anatomy (DA2, Estelite Omega, Tokuyama Dental America).
Conclusions
In order to make the margins of the restoration blend with the natural tooth structure, it is suggested to smooth out the rough, fractured enamel prisms with a long, wavy bevel; etch and bond beyond the bevel; place the dentin composite beyond the dentin/enamel margin; and use an oxygen-inhibited gel for the final curing. These simple techniques created an improved esthetic outcome ad a satisfied and smiling patient.
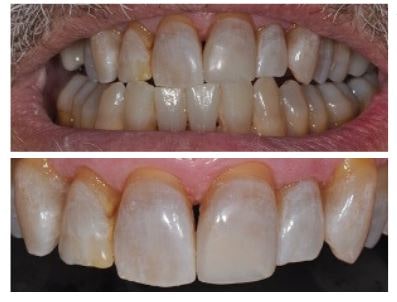
The definitive restoration demonstrates excellent integration of the natural tooth structure and composite restorative material.











